Effective Communication in Healthcare
 There is little debate across industries regarding the power of effective communication. From increased workplace engagement to improvements in collaboration, morale, and overall productivity, everyone wins when we communicate effectively in our personal and professional lives. And when it comes to healthcare, effective communication enhances patient outcomes.
There is little debate across industries regarding the power of effective communication. From increased workplace engagement to improvements in collaboration, morale, and overall productivity, everyone wins when we communicate effectively in our personal and professional lives. And when it comes to healthcare, effective communication enhances patient outcomes.
“In one study using six years of data from nearly 3,000 acute care hospitals, researchers determined that communication between caregivers and patients has the largest impact on reducing readmissions. Specifically, the results indicate that a hospital would, on average, reduce its readmission rate by 5% if it were to prioritize patient communication in addition to complying with evidence-based standards of care.”1
But what happens if your patients don’t speak English? How do you communicate effectively with your limited-English proficient (LEP) patient population? The answer lies in three words — professional healthcare interpreting. By investing in healthcare interpreting, hospitals improve LEP patient outcomes, reduce 30-day readmissions, and shorten the length of hospital stays.
The Benefits of Healthcare Interpreting
Perhaps one of the best known examples of how healthcare interpreting improves patient outcomes was a 3-year study conducted within a US-based tertiary care hospital. The study’s results clearly showed that healthcare interpreting helps to significantly decrease both the length of stay and 30-day readmission rates for the LEP patient population.
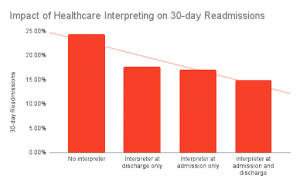
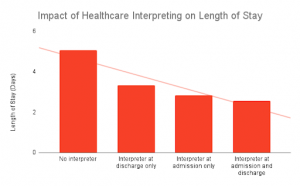
Data Source: US National Library of Medicine2
In fact, the study showed that LEP patients who did not receive healthcare interpreting services had an average increase in their length of stay of 1.11 days and an average increase in their 30-day readmission by almost 39 percent. At the best of times, healthcare interpreting improves patient outcomes, and in emergencies, this service can literally help to save lives.
The Critical Need for Healthcare Interpreting During COVID-19
At the time of this publication, COVID-19 is once again wreaking havoc throughout the United States. In fact, the Centers for Disease Control (CDC) are classifying the entire country (except for a choice few states) as having high community transmission3. Hospitals throughout the nation are once again filled (or rapidly filling) to capacity and are in desperate need of assistance. Not only are healthcare workers struggling to keep up with the daily influx of COVID-19 patients, but in a country with a growing limited-English proficient (LEP) population4, medical staff urgently need healthcare interpreting services to help save lives. One need look no further than the recent 2020 Census to see how the nation’s demographics are becoming increasingly more diverse, heightening concerns about language access for LEP patients.
Linguistic and Cultural Diversity and its Impact on Healthcare
The federal government uses the Diversity Index (DI) to “measure the probability that two people chosen at random will be from different race and ethnicity groups.”5 In 2010, the average DI index throughout the country was 54.9 percent. In 2020, this jumped to a probability of 61.1 percent. To put this into clearer focus, the United States is now home to roughly 67 million residents who speak a language other than English (LOTE) at home and nearly 30 million residents who struggle when communicating in English. In such a linguistically and culturally diverse nation, healthcare interpreting must be an active and ongoing service available throughout the country even outside of public health crises. But, as the U.S. News puts it, “[t]he coronavirus pandemic is intensifying language access issues in healthcare — problems that could be putting both patients and interpreters, as well as the broader public, at risk.”6
Thankfully, with a growing number of interpreting options now available, healthcare facilities throughout the nation can operate in compliance with language access laws and ensure patients’ rights are protected. But how do healthcare facilities decide which form of interpreting to use — in-person, over-the-phone, or virtual remote interpreting (VRI)? Although all three options provide a much needed service with plenty of benefits, the choice is often assessed on a case-by-case basis.
Types of Healthcare Interpreting
In-person Interpreting
Before the onset of COVID-19, in-person interpreting was certainly the preferred method of healthcare interpreting services. In fact, it still is for a great many reasons. The ability to be physically present with the healthcare provider and the patient allows the interpreter to have both visual and auditory proximity. It also provides the interpreter the opportunity to pick up on facial expressions and body language. By its very nature, in-person interpreting also strengthens trust with the patient which can lead to better overall communication.
Over-the-phone Interpreting
Over-the-phone is one popular alternative to in-person interpreting, especially when hospitals limit the number of patient visitors. Since phones are almost always readily available, hospitals, regardless of their location, can seamlessly — and quickly — connect to a much larger pool of interpreters, including interpreters who specialize in rare languages. And, in times of public health crises, this is certainly a very welcomed service. Nonetheless, it is important for healthcare providers and patients alike to consider the lack of visibility which could negatively impact the interpreting experience for all.
Virtual Remote Interpreting
Virtual Remote Interpreting (VRI) is a quickly emerging technology that a growing number of healthcare facilities are now embracing. Ideal for times such as these, VRI is economical, relatively easy to use, and provides almost immediate access to a global network of healthcare interpreters specializing in hundreds of languages. With VRI, all parties can clearly see and hear one another. And although remote, the interpreter can still look for facial expressions as well as body language to gauge a better understanding of how the patient is feeling.
Language Access in Healthcare — Executive Order 13166
In addition to the desire for healthcare facilities to provide the highest level of medical care for all patients, there is another reason to invest in healthcare interpreting. Executive Order 13166, otherwise known as “Improving Access to Services for Persons with Limited English Proficiency”, went into effect in 2020. The order requires any agency receiving federal funds to provide meaningful language access to LEP recipients of any federally-funded service. Since almost 40 percent of Americans are covered by a public health insurance plan7, and since the vast majority of hospitals throughout the United States receive federal funding (at least in part), it is incumbent upon healthcare facilities to comply with the law.
CommGap Specializes in Healthcare Interpreting
With a team of in-house and global employees as well as an extensive network of contracted healthcare interpreters, CommGap offers in-person, over-the-phone, and virtual remote interpreting in over 200 languages. Available 24/7/365, our linguists are specialists in their respective fields, are fully HIPAA-compliant, and undergo ongoing, rigorous industry-specific and cultural-sensitivity training.
As we strive to provide the highest-level of flexible, customizable language solutions to our clients, CommGap offers you the ability to schedule appointments in advance or simply contact us for any last-minute, urgent needs. Our convenient proprietary app, CommGap Connect® will connect you to a healthcare interpreter within seconds. When you want a seamless, end-to-end process for your healthcare interpreting needs, turn to CommGap.
You focus on your patients. We’ll handle the interpreting.
REFERENCES
1 Psqh. “Communication: A Critical Healthcare Competency.” Patient Safety & Quality Healthcare, 19 Dec. 2017, www.psqh.com/analysis/communication-critical-healthcare-competency/.
2 Lindholm, Mary, et al. “Professional Language Interpretation and Inpatient Length of Stay and Readmission Rates.” Journal of General Internal Medicine, Springer-Verlag, Oct. 2012, www.ncbi.nlm.nih.gov/pmc/articles/PMC3445680/.
3 “CDC COVID Data Tracker.” Centers for Disease Control and Prevention, Centers for Disease Control and Prevention, covid.cdc.gov/covid-data-tracker/#cases_community.
4 Griffith, Bryan. “Almost Half Speak a Foreign Language in America’s Largest Cities.” CIS.org, 19 Sept. 2018, cis.org/Report/Almost-Half-Speak-Foreign-Language-Americas-Largest-Cities.
5 Bureau, US Census. “Racial and Ethnic Diversity in the United STATES: 2010 Census and 2020 Census.” Census.gov, 12 Aug. 2021, www.census.gov/library/visualizations/interactive/racial-and-ethnic-diversity-in-the-united-states-2010-and-2020-census.html.
6 “Language Access Issues during Covid-19 Are Proving Dangerous for Some.” U.S. News & World Report, U.S. News & World Report, www.usnews.com/news/healthiest-communities/articles/2020-04-16/language-access-problems-a-barrier-during-covid-19-pandemic.
7 “A Visit to the Doctor’s Office: How the U.s. Government Keeps Americans Safe and Healthy.” House Budget Committee Democrats, 25 Mar. 2020, budget.house.gov/publications/report/visit-doctors-office-how-us-government-keeps-americans-safe-and-healthy.




